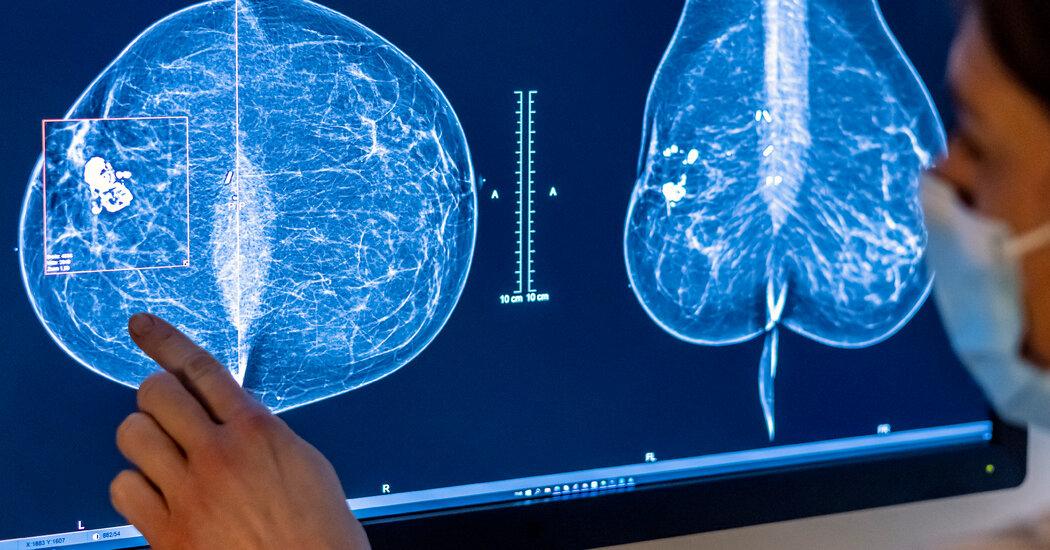
Citing rising breast cancer rates in young women, an expert panel on Tuesday recommended starting regular mammography screening at age 40, reversing longstanding and controversial guidance that most women wait until 50.
The panel, the U.S. Preventive Services Task Force, finalized a draft recommendation made public last year.
In 2009, the task force raised the age for starting routine mammograms to 50 from 40, sparking wide controversy.
The panel continues to recommend screening every two years for women at average risk of breast cancer, though many patients and providers prefer annual screening.
Kathleen Costello, a retiree in Southern California who was diagnosed with breast cancer in 2017 when she was 59, said she was convinced that mammograms missed her cancer for many years.
The letters also told her that she had dense breast tissue and that additional screening was available but not covered by insurance.
or ultrasound, reduces breast cancer progression and extends life for women with dense breast tissue.
For women with dense breasts who are at average risk of breast cancer, recent research indicates that M.R.I.
An expert panel on Tuesday recommended beginning routine mammography screening at age 40, overturning long-standing and contentious advice that most women wait until 50, citing rising rates of breast cancer among young women.
The panel that the U. S. The Preventive Services Task Force completed a draft recommendation that was made available to the public the previous year. The organization offers well-respected counsel on preventive healthcare, and most Americans follow its recommendations.
Widespread controversy followed the task force’s 2009 decision to raise the age at which routine mammograms should begin from 40 to 50. Researchers at the time worried that early screening would have the opposite effect of intended benefits, causing younger women to undergo needless treatment. They also worried that worrying results might result in invasive procedures that cause anxiety in patients, even though they are ultimately unnecessary.
However, according to Dr. John Wong, vice chair of the task force, the number of women in their 40s who have breast cancer is rising, rising by 2% annually between 2015 and 2019. While many patients and providers prefer annual screening, the panel still recommends screening every two years for women at average risk of breast cancer.
“We should recommend screening every other year at age 40 for all women in this country to help them live longer and have a better quality of life because there is clear evidence that it provides sufficient benefit,” stated Dr. Wong, director of comparative effectiveness research at the Tufts Clinical Translational Science Institute and a primary care clinician at Tufts Medical Center.
Representatives Debbie Wasserman Schultz, a Democrat from Florida, and Rosa DeLauro, a Democrat from Connecticut, among other prominent women’s health advocates, have sharply criticized the recommendations, claiming they fall short.
They complained about the guidelines’ continued failure to “fall short of the science, create coverage gaps, generate uncertainty for women and their providers, and exacerbate health disparities” in a June letter to the task force. “.
Adding to the already intense debate, the task force stated that additional scans, like magnetic resonance imaging or ultrasounds, should not be recommended for women with dense breast tissue due to insufficient evidence.
This means that because these women are at a higher risk of developing breast cancer in the first place and whose cancers can be missed by mammograms alone, insurers are not required to cover the full cost of additional screening. This group includes about half of all women over the age of 40.
Laws in recent years have mandated that more mammography providers disclose to women the presence of dense breast tissue and the possibility that mammography may not be an adequate screening method for them.
Patients will have to get that information from all mammography centers in the US starting in September.
Physicians frequently recommend “supplementary” or additional scans for these patients. However, these patients often discover that they are responsible for covering all or part of the costs themselves, even in cases where the extra testing is done as part of preventive care, which is required by law to be provided at no cost.
The government health program for senior citizens, Medicare, does not pay for the extra scans. In the private insurance market, coverage varies widely based on a number of factors, including state laws, plan type, and plan design.
A representative for AHIP, the group that represents health insurance companies, Robert Traynham, stated that the panel’s decision to reject the additional scans has important ramifications for patients.
“That implies that there is no requirement to pay for these particular screenings at zero dollar cost-sharing for women with dense breasts,” he explained in terms of coverage.
According to Mr. Traynham, it is not mandated by law for employers to offer health insurance plans that do this, although some may choose to do so.
After receiving a breast cancer diagnosis in 2017 at the age of 59, Kathleen Costello, a retiree from Southern California, expressed her belief that mammograms were missing her cancer for a long time.
Each year, she received a letter stating that she had not been diagnosed with cancer after undergoing screening. The correspondence also informed her that further testing was possible but not covered by insurance, and that she had dense breast tissue.
Her right breast felt stiff, and she informed her doctor of this six months following an unproblematic mammography in 2016. An ultrasound and a mammography were ordered by the doctor.
Ms. Costello stated in an interview that the ultrasound detected the cancer in 30 seconds and that she knew because “the technician blanched and left the room.”. “.
“It’s hard for me to accept that it grew in six months from undetectable to four centimeters,” Ms. Costello continued, describing the size of the mass as four centimeters. “.
However, task force member Dr. Wong asserted that there was no scientific proof that additional imaging, performed by either M.R, was necessary. Me. or ultrasound, prolongs life for women with dense breast tissue and slows the progression of breast cancer.
Contrarily, there is a wealth of evidence indicating that additional screenings could result in biopsies and a high rate of false-positive results, which would increase stress and needless invasive procedures.
Dr. Wong remarked, “It’s tragic.”. We share the same frustrations as women. They are entitled to information about whether further screenings would be beneficial. “.
However, for women with dense breast tissue, additional screening is recommended by medical associations such as the American College of Radiology. According to Dr. Stamatia Destounis, chair of the college’s breast imaging commission, studies have demonstrated that when ultrasound and mammography are combined, they can identify extra cancers in patients with dense tissue.
According to recent research, M.R is associated with an average risk of breast cancer in women with dense breasts. Me. is the greatest supplemental scan, according to Dr. Destounis, “having more favorable positive predictive values and far better cancer detection.”. “.
Additionally, the college suggests yearly screening for women with average cancer risk as opposed to the panel’s recommendation of every two years. In order for women who are at high risk to begin screening even before they turn forty, the group of radiologists is pushing for a recommendation that all women should have their risk of breast cancer evaluated before the age of twenty-five.